Histologic:Chapter 7
Contents
Introduction
The formed elements of blood, which are suspended in the fluid plasma, are: erythrocytes (red blood cells), leukocytes (white blood cells), and platelets. Several methods exist for studying the formed elements of the blood and serve various purposes. Clinically, the type of preparation used most often is the blood smear in which a drop of blood is spread on a slide and then stained, usually with Wright’s stain.
Blood Smears
Slide 37: Blood Smear (Wright's stain)
Examine slide 37. This is a blood smear stained with Wright’s stain. Wright’s stain is a polychrome stain in wide use for fixing as well as staining smears of blood as well as exudates and protozoan parasites. Its staining action depends upon a combination of methylene blue and eosin, which stain both independently as well as synergistically. The solution thus contains three staining factors that color the various structures of the preparation selectively.
At 10x power note that in some areas of the slide the cells (predominantly erythrocytes) are spread far apart and in other areas may be piled on top of one another. In the former area the densely staining white blood cells are flattened out, while in the latter they are more nearly spherical and much smaller. The optimum area for observation is somewhere between these extremes.
In an optimum area, examine the cells at high power.
Erythrocytes (red blood corpuscles)
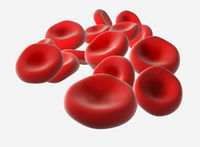
Note the staining, size, and shape of these elements. Erythrocytes are biconcave discs that average 7.7μm in diameter and 1.9μm in the greatest thickness. Look at the scanning EM picture (below) to see the three dimensional appearance of erythrocytes. Adult men have an average of 5.5 million RBCs and 8 thousand white blood cells per cubic millimeter of blood; thus, only one leukocyte exists for every six to seven hundred RBCs.
Crenation of erythrocytes may be observed; this shrunken and indented appearance occurs when erythrocytes are in a hypertonic environment. In a hypotonic solution the erythrocytes may swell and rupture; this process is known as hemolysis. Rouleaux formation is the stacking of erythrocytes.
In certain kinds of anemias the RBCs may be larger than normal (macrocytes) or smaller than normal (microcytes). In normal blood the range in size of erythrocytes is very narrow with the differences in diameter usually being less than one micrometer.
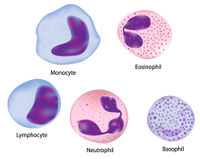
Leukocytes (white blood cells)
Leukocytes are divided into two major types: the granulocytes and the agranulocytes. The white blood cells are involved in inflammatory and immune reactions and function both within and outside of the bloodstream. In different disease states a marked increase in numbers of leukocytes above the normal range is called leukocytosis (10,000 or more per cu. mm) whereas a decrease below 5000 per cu. mm is called leukopenia.
Granular leukocytes (granulocytes) are the leukocytes that contain specific cytoplasmic granules, and they usually have a lobed nucleus. Because of this nuclear feature the granulocytes are often spoken of as being polymorphonuclear leukocytes. However, keep in mind that most hematologists and medical technicians use the terms “polymorphs” or “polys” for just the neutrophils. Although sometimes appearing separated from each other, the nuclear lobes are actually connected by thin delicate strands of nuclear material.
Neutrophils
In the normal, healthy individual neutrophils are the most common the leukocytes, making up 50 - 75% of the white blood cells. Between 3,000 and 6,000 neutrophils per cubic mm make up the normal range. They average 9 - 12 μm in diameter, usually contain 3 - 5 nuclear lobes and possess neutrophilic and azurophilic granules.
Study various neutrophils noting their size, shape, staining features, granularity, and nuclear configuration. Look for neutrophils with various numbers of nuclear lobes. The neutrophils with nonsegmented nuclei (“band forms” or “stabs”) in which the nucleus is simply elongate and/or horseshoe- shaped are younger cells than those in which the nucleus is differentiated into three, four or five lobes.
In approximately 3% of the neutrophils of females a nuclear appendage, like a small “drumstick” is present. This represents the inactive X sex chromatin comparable to the Barr body found in buccal smears and other cells.
Neutrophils act as the first line of defense against many invading organisms. We sometimes speak of neutrophils as being the tissue microphage since they mainly serve to phagocytize bacteria and small particles as compared with macrophages, which ingest much larger particles.
Eosinophils
These granulocytes constitute 2-4% of the leukocytes. They are close to the same size as the neutrophils or just slightly larger (10-15μm in diameter). Characteristic features of eosinophils include large coarse eosinophilic granules and a bilobed nucleus (usually). Eosinophils are important in engulfing antigen-antibody complexes. They increase markedly following certain allergic reactions and parasitic infestations. The eosinophilic granules function as large lysosomes; they give positive reaction for the common lysosomal enzymes and for peroxidase.
Basophils
Basophils are smaller than the other granulocytes being only 8- 10μm in diameter, and they are fewer in number making up only 0.5 to 1% of the leukocyte population. These cells are easily recognized in Wright-stained blood smears because of their coarse, large basophilic granules. These large, dark purplish granules may cover the nucleus that is often elongated and folded in the form of a “U” or an “S.” Basophils carry heparin and histamine in their granules.
Agranular Leukocytes
Agranular leukocytes (agranulocytes or round cells), are leukocytes that lack specific granules, although a few inconstant, non-specific granules do occur in the cytoplasm. The latter are mainly of lysosomal nature. Lymphocytes and monocytes make up the agranular leukocyte population of white blood cells.
Lymphocytes
In normal circulating blood 20 to 40% (1,000 to 3,000 per cu. mm) of the leukocytes are lymphocytes with the average being about 25%. In blood smears the small lymphocyte has an average diameter of 7-8μm with the size range being between 6-10μm. Traditionally, lymphocytes in blood have been considered as small, medium, and large. The latter are very difficult to distinguish from monocytes.
Two distinct populations of small lymphocytes occur in the blood stream (the T and B lymphocytes), but they cannot be distinguished on a morphological basis. However, they do differ in developmental background, in life span, and in their defensive roles in the immunological responses of the body.
Note the size, shape, and comparative numbers of the lymphocytes on your slide. Compare their size with nearby erythrocytes. The nucleus is nearly spherical or slightly indented, dense, dark and it is usually surrounded by a thin rim of basophilic-staining cytoplasm. The coloration of the cytoplasm in high quality Wright’s stained smears ranges from a clear blue color to a greenish blue.
Monocytes
This is the largest of the leukocytes. It ranges between 12 and 20μm and makes up 3-8% of the white cell population in a blood smear. It is often difficult to distinguish clearly between a monocyte and a large lymphocyte. Monocytes rarely have a spherical nucleus like the lymphocyte. Instead, the monocyte nucleus is usually oval or it is indented or horseshoe- shaped. Also, it tends to be eccentrically located and it stains lighter than the lymphocyte nucleus because the chromatin is less dense. Often the nucleus appears “wrinkled,” twisted or folded, and not as uniformly stained as the lymphocyte nucleus.
With Wright’s stain the cytoplasm is a grayish blue or a “muddier blue” than the lymphocyte cytoplasm. Nonspecific, azurophilic granules (lysosomes) occur in the monocyte cytoplasm.
Monocytes give rise to tissue macrophages. The average time spend in the blood stream for a monocyte is three days. Monocytes originate from stem cells in the red bone marrow.
Study the monocytes on your slide noting size, shape, granularity, and the coloration of the cytoplasm and nucleus.
Platelets
These are ovoid to round cytoplasmic fragments (not cells) derived from megakaryocytes of red bone marrow. Platelets average 3μm in diameter and number 200,000 to 300,000 per cu. mm. In blood smears platelets tend to clump together so they are difficult to count accurately. In making counts of platelets it is essential to draw the blood into a syringe or pipette containing antiagglutinins. Platelets function in agglutination (the clumping of platelets in flowing blood) by adhering to the injured walls of blood vessels. From this action the coagulation of blood occurs in which a meshwork of fibrin materializes and the blood becomes clotted.
The basophilic staining central region of a platelet is called the granulomere or chromomere because the cytoplasm here contains more granules and organelles than the peripheral cytoplasm, which is pale and homogenous. This thin peripheral zone of cytoplasm is called the hyalomere. It stains a pale blue. The characteristic granules of human platelets, called alpha granules, are approximately 0.2μm in diameter. The currently known list of alpha-granular proteins continues to enlarge and includes many adhesive proteins (e.g. Fg, von Willebrand factor (vWf) and thrombospodin (TSP)), plasma proteins (e.g. IgG and albumin), cellular mitogens (e.g. platelet derived growth factor and TGF beta), coagulation factors (e.g. factor V) and protease inhibitors (e.g. alpha 2-macroglobulin and alpha 2-antiplasmin). More recently the inner lining of the alpha-granule unit membrane has been demonstrated to contain a number of physiologically important receptors including glycoprotein IIb/IIIa (alpha IIb beta 3) and P-selectin.
Slide 8: Intervertebral Disc (H&E)
On slide 8, Intervertebral disc (H&E) find the red bone marrow and identify the megakaryocytes from which platelets are derived. Megakaryocytes are the largest cells found in normal bone marrow. The nucleus is multilobed and polyploid since chromosomal replications occur in these cells without cytoplasmic divisions.
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||