Histologic:Chapter 17
Contents
Introduction[edit]
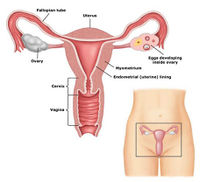
The female reproductive system consists of the ovaries, the two uterine tubes (oviducts or Fallopian tubes) a uterus, a vagina, the external genitalia and the mammary glands. Normally, the development of this system requires that the zygote have the XX sex chromosomal complement. The ovaries produce the ova or female germ cells and certain hormones; the uterine tubes are necessary for transporting sperm to the ova for fertilization and for transporting the zygote to the uterus. Growth and maturation of the conceptus occur in the uterus. The vagina and external genitalia are the copulatory organs and the mammary glands serve for nutrition of the newborn.
Ovary[edit]
With the exception of slide 255, Monkey ovary (PASH), all other slides were obtained from human sources.
Study first slide 255 since it shows all the representative stages of follicle development. Then study slide 251, Ovary, (H&E); it has very small normal follicles, larger atretic follicles and corpora albicantia. Slide 254 Ovary (Masson) shows a large well-developed corpus luteum and a small atretic follicle with a prominent glassy membrane.
Slide 255, Ovary (PASH)[edit]
Slide 255, Ovary (PASH) shows a mature ovary with one large corpus luteum, several large preovulatory follicles, smaller growing follicles, and atretic follicles. Only a portion of the whole ovary is on the slide.
Study the cortex of the ovary.
Identify the surface epithelium (germinal epithelium), the tunica albuginea (a zone immediately beneath the surface epithelium which is more compact and less cellular than the stroma) and the stroma of cellular connective tissue.
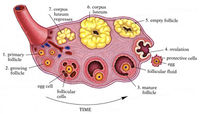
Study the various stages of follicles.
Primordial (unilaminar follicles) consists of a small primary oocyte surrounded by a single layer of squamous follicular cells which rest on a basement membrane.
A primary follicle contains an enlarging oocyte surrounded by a single layer of flattened, cuboidal or low columnar follicular cells. These cells give rise to granulosa cells by mitosis.
Growing or multilaminar follicles are surrounded by several layers of follicular cells.
Vesicular (secondary or antral) follicles consist of a primary oocyte surrounded by 6-12 layers of granulosa cells. Fluid-filled spaces that appear between the granulosa cells gradually enlarge, interconnect, and eventually form a crescent-shaped cavity, the antrum.
Note the PAS-positive staining basement membrane located between the outer row of granulosa cells of the follicle and the stromal cells. Observe that the stromal cells are organized as a sheath of cells around the growing follicles.
The vesicular follicles are surrounded by a stromal sheath called the theca folliculi; the theca is divided into two regions, a theca interna and a theca externa.
The theca interna is a zone of epithelioid stromal cells surrounding the outer granulosa cells but separated from them by the basement membrane; this portion of the theca is vascular, containing capillaries and smaller blood vessels.
The theca externa lies external to the theca interna and consists of condensed stroma.
As the follicle enlarges, so does the oocyte. Increase in volume of both the nucleus and the cytoplasm accounts for oocyte enlargement. Observe the prominent nucleolus and the nuclear membrane of the oocytes; note that the cytoplasm is weakly acidophilic.
The zone pellucida is a prominent PAS-positive staining membrane immediately surrounding the oocyte’s plasma membrane. It is not present in primordial follicles or in smaller growing follicles.
The degeneration of follicles is called atresia and signs of this activity can be identified as follows:
- The granulosa cell layer may be partially detached from the theca interna.
- Groups of cells with pyknotic nuclei appear in the granulosa layer.
- Fragmentation of the oocytes may be occurring.
- The oocyte nucleus may be pyknotic (highly condensed and dark staining).
- The basement membrane is very irregular, wavy, and fragmented.
- The zone pellucida is fragmented or broken in places.
Study the vesicular (secondary or antral) follicles.
Identify early antrum formation in which the follicular cavity is small. Call-Exner bodies may be present between granulosal cells; they are strongly PAS-positive.
Find a large follicle (large antrum) in which the large volume of the antrum indicates it is filled with fluid called liquor folliculi.
The cumulus oophorus is a mound or hill of granulosa cells surrounding and supporting the large oocyte. This structure is present in the mature (Graafian) follicle.
The corona radiata is a cluster of granulosal cells which immediately surrounds the zona pellucida. When the ovum breaks free from the cumulus oophorus the corona radiata cells “go with it” and surround the ovum during ovulation and transport into the uterine tube.
Recall that just prior to ovulation, the primary oocyte undergoes its first maturation division, giving off the first polar body, to form a secondary oocyte. The final maturation division will not occur unless fertilization ensues.
Study the corpus luteum.
A corpus luteum is a new endocrine organ that makes its appearance after ovulation. The granulosa cells of the follicle hypertrophy, become luteinized and form granulosa lutein cells which secrete primarily progesterone. The corpus luteum on this slide is in an early stage of development. Note its large size. It consists of a thick folded wall and a central cavity (the former antrum of the follicle) which is filling in which fibrin deposits and loose connective tissue growing in from the theca externa.
Most of the wall is composed of granulosa lutein cells derived from the granulosa cells of the mature follicle. They are large cells with pale cytoplasm and a vesicular nucleus containing a prominent nucleolus. The cell membrane is stained with PAS. The cells are packed closely together, but fibroblasts, fine connective tissue, and capillaries invading from the stroma are penetrating between the cells toward the central cavity.
The theca lutein cells form a thin zone at the periphery of the corpus luteum and extend into the folds (which were formed when the ruptured follicle collapsed). They are not too apparent with this stain, but they are smaller cells than granulosa lutein cells.
The former antrum has fibrin deposits and is filling in with loose connective tissue.
The remains of atretic follicles can be seen as small irregular, intensely stained PAS-positive structures that are hypertrophied zona pellucida remnants from atretic follicles. They may or may not be surrounded by a greatly thickened folded glassy membrane (basement membrane) which stains pink. Both structures will be replaced by stroma.
Study the medulla of the ovary.
The medulla contains fibroelastic tissue, many large and smaller vessels, nerves, and lymphatics. Most of the blood vessels are highly coiled or convoluted.
The medulla is continuous with the connective tissue of the mesovarium, a short peritoneal fold that attaches the ovary to the broad ligament; the point of attachment serves as a hilus for the ovary. The mesothelium of the serosa (visceral peritoneum) of the mesovarium is continuous with the surface epithelium of the ovary.
A homologue to the rete testis in the male, the rete ovarii, can be seen in one part of the medulla (upper left in the field). They are distinguished by small, deeply basophilic nuclei of cuboidal cells lining an irregular-shaped lumen.
Slide 251, Ovary, Human (H&E) (From an elderly woman)[edit]
Study the cortex of this ovary.
Note the prominent tunica albuginea just underneath the surface epithelium. The single layer of simple cuboidal cells making up the surface epithelium is present only in patches since part of it was sloughed off during preparation of the tissue.
The stroma is much more evident on this slide as compared with the monkey ovary just studied. Note the swirling pattern of the stromal cells, especially how they begin to swirl and encircle a follicle some distance from the follicle. In growing follicles, the stromal cells begin to condense into the thecal follicular sheath of cells that contribute to the function of the follicle.
Find primordial, primary and small growing follicles; (Primordial follicles are rare in mature ovaries). Note those follicles that show signs of atresia.
The two or three large follicles (preovulatory follicles) on this slide are also in early atresia. Granulosa cells have sloughed off or are still sloughing; the basement membrane in one follicle is beginning to hypertrophy.
Look for parts of corpora albicantia (singular = corpus albicans) which are fibrous scars that replace regressed corpora lutea; they are composed of compact collagenous fibers and fibroblasts, and have indefinite borders which merge with the stroma
Study the medulla of this ovary.
Note numerous, prominent blood vessels of various caliber which take up most of the volume of the medulla. Some of these vessels are quite convoluted (a long row of cross-sections of a vessel, each cross-section of about the same diameter, may be observed.
Lymphatics are also a prominent feature of the ovarian medulla. They are more difficult to distinguish because their thin walls may have collapsed, eliminating the lumen.
Vasomotor nerves to the smooth muscles of blood vessels may be seen; they are too small to see clearly.
Slide 254, Ovary, Human (Masson)[edit]
The principal structure occupying most of this section is a corpus luteum. Other follicles may also be present, but concentrate on the corpus luteum.
The corpus luteum represents a very young stage of development, soon after ovulation. The amount of connective tissue located in the middle of the corpus luteum indicates the age of the organ. Note the huge size of the corpus luteum; it occupies most of the section.
Observe again that granulosa lutein cells make up the bulk of the corpus luteum; these are large cells with granular cytoplasm, vesicular nuclei and prominent nucleoli. Due to artifact of preparation or postmortem changes the cells are separated from each other by spaces.
The granulosa lutein cells are arranged into groups separated by delicate strands of connective tissue and capillaries.
In the central cavity are strands of clotted blood (red blood corpuscles and precipitated fibrin) and fine fibrin filaments. Little or no connective tissue is present as yet.
Numerous dilated blood vessels are seen in the stroma around the periphery of the corpus luteum, probably still in this state from their preovulatory condition.
The blue-staining connective tissue on the outer margin of the corpus luteum represents the former theca externa.
Theca lutein cells are present on the periphery and in the folds of this corpus luteum but are not yet well differentiated, thus are not easily identified. Blood vessels and connective tissue will be growing in from the former theca externa.
If fertilization does not take place, the corpus luteum persists for about two weeks, and then it breaks down (regresses) to become a corpus albicans. The corpus luteum in this case is called a corpus luteum spurium (false) or corpus luteum of menstruation.
If fertilization occurs, the corpus luteum persists, gets larger, and lasts longer; it is now called a corpus luteum verum (true) or corpus luteum of pregnancy.
Uterine Tube[edit]
Each uterine tube is about 12 cm long and serves to connect the uterus with the ovaries for transport of spermatozoa, fertilization of the ovum and nourishment and transport of the zygote. The uterine tube is embedded in (courses through) the mesosalpinx which is the upper part of the broad ligament of the uterus. Within this mesentery of the uterine tube is a central core of connective tissue, some smooth muscle, blood vessels and nerves, and it is covered by a serosa (peritoneum). Thus the wall of the uterine tube consists of three layers: a mucosa, a muscularis and a serosa.
Four regions of the uterine tube are generally recognized; from the uterus distally they are the interstitial (intramural) segment, the isthmus, the ampulla and the infundibulum. Only two regions or segments are represented in these slides. These are slides of the ampulla (slides 256, 257 and 258 and of the isthmus (slide 259).
Slide 257, Uterine Tube Ampulla (Masson)[edit]
Study the mucosa (mucous membrane) of this section of the uterine tube; note the complex foldings of the mucosa. The epithelium is actually simple columnar, but it frequently appears pseudostratified. It is tallest in the ampulla and decreases in height towards the uterus.
The epithelium consists of two types of cells, ciliated columnar cells (numerous on the fimbria and in the ampulla) and non-ciliated columnar secretory cells (peg cells).
The thin lamina propria is a primitive type of connective tissue, quite cellular; it extends into the folds. It is loosely arranged in the ampulla and is quite vascular. (It undergoes a decidual reaction, resembling decidual stromal cells found in the endometrium of the pregnant uterus, when tubal pregnancy occurs).
Observe the muscularis (muscular coat). It has two ill-defined smooth muscle layers; the inner spiral circular layer is thicker than the outer longitudinal muscle layer. Fine connective tissue intermingles with smooth muscle cells.
Surrounding the muscularis and intermingling with it is vascular connective tissue of the mesosalpinx. Note here the numerous greatly congested blood vessels of various diameters. Such congestion usually indicates a preovulatory state. A serosa forms the outermost layer.
Slide 258, Uterine Tube, Ampulla (PASH)[edit]
This section of uterine tube is also from the ampulla in a pre-ovulatory state.
The two epithelial cell types can be identified; there appear to be fewer ciliated cells (may be post-mortem loss). PAS clearly demonstrates basement membranes of the epithelial cells as well as elastic membranes in blood vessels.
In the lamina propria, the looseness of the connective tissue in the folds is better demonstrated than in slide 257. Note branched fibroblasts and scattered lymphocytes. Lymphocytes may also be seen migrating through the epithelium to be eliminated from the body. Many dilated blood vessels are seen in this region.
The muscularis appears as patches of smooth muscle fibers dispersed among a loose arrangement of connective tissue fibers. Numerous dilated blood vessels are interspersed in the connective tissue among the bundles of muscle fibers.
Slide 256, Uterine Tube (Ampulla) of Pregnancy (Masson)[edit]
This section represents uterine tube removed from a pregnant woman. There are artifactual breaks in the tissue section.
Identify the cell types in the epithelium. Nonciliated peg cells are most predominant, but this varies from place to place. The connective tissue of the lamina propria has proliferated to appear more like a primitive connective tissue; lymphocytes are more numerous. In the connective tissue you may be able to see large, pale-staining decidual cells which look like macrophages. These are glycogen storing cells that occur in great numbers in the uterus during pregnancy.
Lymphocytes, decidual cells, and other cells appear to be working their way between the epithelial cells into the lumen, probably a reaction to an interrupted pregnancy. They are surrounded by a vacuole.
Identify the layers of smooth muscle forming the muscularis, the numerous blood vessels in the connective tissue between the muscle bundles, and serosa covering most of the section.
Slide 259, Uterine Tube (Masson)[edit]
This section is from the isthmus segment of the uterine tube, which lies along the uterine wall. Compare with slide 257, ampulla.
Observe the size of the lumen, the degree of mucosal folding, the height of the epithelium and the width of the lamina propria and the muscularis. The mucosal foldings are much less complex than in the ampulla.
Due to the thickness of this section of uterine tube its epithelium appears to be pseudostratified tall columnar. The nuclei are elongated and a few cells appear ciliated.
The lamina propria is more compact in the isthmus than in the folds of the ampulla.
Compare this section with that of the ductus deferens (slide 232) with which it might be confused. One should be able to distinguish them by the epithelium and by the layers of muscle.
Uterus[edit]
The uterine slides demonstrate two phases of the menstrual cycle and one of pregnancy. No slides are available from premenstrual and menstrual phases of the uterus.
Slide 278 (H&E) is from the early proliferative phase.
Slide 261 (H&E) is from the proliferative phase.
Slide 262 (H&E) is from the secretory phase.
Slide 264 (PASH) is from pregnant uterus; it shows decidual cells in the stroma and also has some placenta attached to it.
Slide 278, Uterus, cross-section (H&E)[edit]
Slide 278, Uterus, cross-section (H&E), shows endometrium in early to mid- proliferative phase of the menstrual cycle (days 7 to 9).
Identify: endometrium (mucosa), myometrium (muscularis), and perimetrium (serosa).
Study the endometrium.
Distinguish two zones in the endometrium:
- The basalis (deep layer) where the stroma is compact and glands are branched.
- The functionalis, the entire endometrium above this. The stroma is not as compact as in the basal layer, but is quite dense in comparison with endometrium in later phases of the cycle.
Note the simple columnar surface epithelium; it may appear pseudostratified but all nuclei are similar, therefore all cells are columnar. Occasional lymphocytes lying in a small vacuole are seen in the columnar cells.
Simple tubular glands indent from the surface epithelium and extend through the thickness of the endometrium, becoming branched in their deepest parts. Some glands may extend into the myometrium for a short distance. The glandular epithelium is simple columnar that may also appear pseudostratified. Cytoplasm is very granular. Nuclei are basally located. Epithelium is proliferating; look for mitotic figures.
The stroma is a “cellular” connective tissue, with fibroblasts with large oval nuclei and branching cell processes embedded in fine collagenous and reticular fibers. It resembles embryonic connective tissue. Some proliferation of fibroblasts is still in progress; look for mitotic figures. Some lymphocytes are present, especially in the most peripheral stroma. Note that the stroma is denser in the basal layer. This region remains relatively inactive.
Look for coiled arteries in the lower fourth or third of the endometrium. Later, they will extend almost to the surface. A group of cross sections of these arterioles or very small arteries represents one coiled artery. Capillaries and venules are throughout the endometrium.
Myometrium (muscularis).
Note the thickness of the myometrium and the density of the muscle. Attempt to define the three layers of muscle but in a section it is difficult to do so.
Stratum subvasculare, adjacent to the endometrium. Muscle fibers are in compact bundles, in cross or oblique sections (course longitudinally in the intact uterus), with prominent septa between them.
Stratum vasculare, the middle layer, the thickest part of the muscularis. Interlacing bundles of muscle course both circularly and spirally.
Note the large blood vessels in the deeper part of this stratum. Their peculiarities are normal for the uterus. These include muscle in the intima of the arteries, increased muscle in the media of the veins, and sometimes muscle in the adventitia of both. (Some arteries in this slide have arteriosclerosis or intimal hyalinzation.)
Stratum supravasculare, the thin most peripheral layer, with longitudinal and circular fibers.
Perimetrium (typical serosa): mesothelium and a little underlying loose connective tissue.
Slide 261, Uterus (H&E)[edit]
Slide 261, Uterus (H&E), later proliferative phase, probably about days 10-12.
Study the endometrium in comparison with slide 278.
Note that the endometrium is a wider layer.
Stroma is much less compact - more tissue fluid is present, fibroblasts are farther apart. Nearer the epithelium, stroma in places is beginning to have a spongy appearance.
Glandular cells are larger, nuclei are large and vesicular, and epithelium appears pseudostratified. Secretion (glycogen, mucin) is beginning to accumulate at the bases of many cells. Small vacuolated areas represent the secretions that are removed during section preparation.
Fibroblasts are seen more distinctly in the looser stroma; note their processes. Look for mitoses. Small lymphocytes are scattered throughout.
Look for coiled arteries but they are not too prominent on this slide. Look for other small blood vessels.
Slide 262, Uterus (H&E)[edit]
Slide 262, Uterus, (H&E) exhibits endometrium in a very late secretory phase or early premenstrual (probably days 24-26 of cycle; it is difficult to date precisely).
Study the endometrium of this phase of the uterine cycle.
Compare the width of the endometrium in this phase of the cycle with that in the previous slide.
Note the characteristic large sacculated glands (“corkscrew appearance”). These are prominent throughout most of the functional zone. In the upper region of the functionalis zone (towards the surface) the glands have larger lumina but the sacculations in the walls are less.
Note the position of the nuclei and the size of the glandular cells. Secretory material has moved from the infranuclear position to the supranuclear position, and some secretion has been liberated into the lumens of the glands. Therefore, the cells are smaller than in the earlier secretory stages, pseudostratification is much less apparent, and nuclei are basally located.
Note areas of edema in the functional zone, but much of the excessive tissue fluid has already been resorbed.
Note now the large size of the coiled arteries and their extent halfway or more upward into the functional zone.
Observe the increased vascularity of capillaries and venules, especially in the outer functional zone. Some may already have ruptured.
The surface epithelium is still intact.
Note the myometrium and its blood vessels. Perimetrium is not present.
Slide 281, Cervix and OS Cervix, one wall (H&E)[edit]
Slide shows endocervical epithelium and glands. The plane of section missed the junctional zone between endocervix and os cervix.
Locate the os cervix (portio vaginalis) which is lined with stratified squamous epithelium. It can be seen grossly on the right margin of the section.
Look along either surface of the section for cervical mucosa. The simple columnar lining epithelium consists of tall columnar cells, mucus-secreting; the luminal margin of the cells often appears indistinct or ragged. Note the Nabothian cyst (a cyst of a mucous gland of the cervix).
The surface epithelium continues down to line the simple branched tubular mucus-secreting cervical glands.
The lamina propria is no longer a primitive connective tissue as in the uterine endometrium.
The mucosa is often folded, forming plicae palmatae.
Vagina[edit]
The vagina is a thick-walled fibromuscular tube that connects the uterus with the exterior and serves as a cavity for the reception of the penis at coitus and as a birth canal at the time of parturition.
Slide 266, Vagina (H&E)[edit]
The wall of the vagina consists of a mucosa, a muscularis, and a broad fibrosa that connects it to adjacent structures. The mucosa is thrown into broad folds (rugae) which are gross structures, not demonstrable in a small piece of tissue used for microscopic slides.
Mucosa
The epithelium is non-cornified stratified squamous. Note the stratum basale, the stratum spinosum, and the stratum corneum, so-called even though it is not cornified. The cells that appear empty contain glycogen and mucin, both of which are removed during routine section preparation.
The broad areas of epithelium are tangential sections. Cross-sections of connective tissue papillae may be seen within them.
Note connective tissue papillae projecting into the epithelium from the lamina propria. These are characteristic of most stratified squamous epithelia.
The lamina propria is a broad zone of highly vascularized connective tissue, with abundant elastic fibers, extending to the muscularis. The elastic fibers may be seen as fine homogenous threads. (There is no muscularis mucosae or submucosa.) Note numerous small blood vessels and nerves. In many of the vessels, the endothelial cells (nuclei) are hypertrophied - not a normal condition.
Scattered lymphocytes and plasma cells are seen throughout the mucosa. Lymphocytes may aggregate just below the epithelium to form diffuse lymphatic tissue or an occasional small nodule. Lymphocytes may penetrate the epithelium to migrate toward its surface.
The muscularis, mostly arranged longitudinally, appears as bundles of smooth muscle interspersed with connective tissue rich in elastic fibers which may be seen as thin, homogenous threads. Larger blood vessels, as well as small ones, are found in the deep muscularis or fibrosa.
The fibrosa is loose connective tissue. It should have some adipose tissue and nerves.
Slide 265, Vagina (Masson)[edit]
Identify the regions of the wall and their component parts as in slide 266.
Muscle and connective tissue are easily differentiated with Masson’s; they stain red and blue respectively. All nuclei stain red, as do erythrocytes. Elastic fibers are not distinguishable.
The vascularity of the lamina propria is emphasized, with many of the venules congested.
The large amount of connective tissue between the muscle bundles is well demonstrated.
Lightly staining nerves occur among the muscle bundles and in the fibrosa.
Placenta and Umbilical Cord[edit]
Slides: 275, 264, 273, 274, 279, 280.
Slide 275, Chorionic Villi (H&E)[edit]
This is a section of a small part of a fetal placenta of a very early pregnancy, showing chorionic villi and the surrounding maternal blood spaces. Some slides have a strip of chorionic plate across the upper margin of the section.
Chorionic plate
The greater part of the plate is chorion, composed of a mass of embryonic connective tissue (large fibroblasts, fine collagenous fibers, abundant ground substance), covered on its lower surface by a double layer of epithelial cells: the cytotrophoblast adjacent to the connective tissue, and the syntrophoblast (syncytial trophoblast) on the free surface, bordering on maternal blood spaces.
Cells of the syntrophoblast do not show cell boundaries. Ragged cell surfaces indicate microvilli. Cells of the cytotrophoblast supposedly show cell boundaries but they are not readily seen here. They divide to form syntrophoblast.
Note blood vessels in the connective tissue (branches of umbilical vessels) containing nucleated fetal red blood corpuscles.
The small zone of looser connective tissue in the upper part of the chorionic plate is part of the amnion. The cuboidal surface epithelium has been torn off.
Chorionic villi. The villi are outgrowths from the chorion, having the same structure as the chorion. They increase in size and branch repeatedly as they invade the maternal blood spaces. The initial larger villi will become the anchoring villi that will penetrate the endometrium (decidua basalis) to anchor the fetal placenta. Smaller villi sprout off the anchoring villi.
Note that the villi vary in size. The largest ones are potential anchoring villi. Others are floating villi; their free ends are in the blood spaces.
Each villus has a core of embryonic connective tissue, branches of umbilical vessels (sparse in this early placenta), and a covering of inner cytotrophoblast and superficial syntrophoblast.
Slide 264, Uterus and Placenta from a later stage of pregnancy (PASH)[edit]
Look at the fetal placenta.
Villi are larger and more numerous than in slide 275, stroma is generally more compact with more collagenous fibers (still fine) and abundant fibroblasts.
Blood vessels in the villi are more numerous. Capillaries and little venules are peripherally located close to the trophoblast cells, although this may not be obvious due to plane of sections. Note that now red blood corpuscles are not nucleated.
Syntrophoblast and cytotrophoblast are still present but cytotrophoblast is incomplete in many areas. (It will disappear entirely by late pregnancy.)
Look for macrophages (Hofbauer cells) in the stroma of the villi - large rounded cells whose cytoplasm may have small vacuoles and/or PAS positive granules.
Look for syncytial knots on the surface of villi or in the intervillous spaces. These are groups of syntrophoblast cells that detach from the villi and float freely in the spaces; progressively more are formed toward term.
Look for very small deposits of fibrinoid, on or in the villi or in the intervillous spaces, a non-cellular, homogenous, proteinaceous material associated with transplantation immunity to protect the fetus.
Maternal placenta (decidua basalis) and uterus. The decidua basalis is the name given to the endometrium that underlies the villi of the fetal placenta. Some villi (anchoring villi) penetrate the decidua basalis (endometrium) for varying distances. In doing so, part of the surface of the endometrium has been eroded and destroyed (surface epithelium is missing).
Look for anchoring villi attaching to the decidua basalis. Note larger fibrinoid deposits and aggregations of syncytial knots in this region.
In the decidua basalis, note the vast numbers of large and smaller decidual cells with PAS- positive cytoplasm (are storing glycogen) and large, lightly staining nuclei. Cytoplasm of those with less glycogen stains faintly acidophilic or somewhat grayish. Decidual cells are derived from fibroblasts of the endometrium.
A few glands are seen in the basal zone of the endometrium. They may be dilated, have very low epithelium or hypertrophied epithelium, and have lymphocytic infiltration surrounding some of them.
Identify the myometrium and note the large size of the muscle fibers that hypertrophy greatly during pregnancy.
Slide 280. Uterus and Placenta near term (H&E)[edit]
Fetal placenta. Proliferation of villi has continued to increase during pregnancy.
Note the great number of chorionic villi, practically filling the maternal blood spaces. The anchoring villi have become very large. The connective tissue in the core is fibrous, but embryonic connective tissue has persisted at the periphery. The larger blood vessels course in these villi. Observe the variation in size of the floating villi, which continue to form throughout pregnancy.
In the villi, note further compactness of stroma, areas of more dense collagenous fibers, more capillaries, and venules close to the trophoblast.
Look for macrophages (Hofbauer cells) in the stroma of the villi. With H&E, the cytoplasm is finely vacuolated.
Syntrophoblasts still cover the surface of the villi. Cytotrophoblasts have generally disappeared.
Note increased number of syncytial knots and much fibrinoid material. Knots are seen deep in the endometrium; they appear as darkly stained groups of pyknotic nuclei.
The maternal placenta (decidua basalis).
Again note the placental villi anchoring into the endometrium.
Decidual cells are still present in the endometrium but many have “used up” their glycogen and are reverting to fibroblasts. Lymphocytic infiltration is seen in places. Much fibrinoid is present.
Uterine glands, whose basal portions had remained inactive, are proliferating and regenerating. Some appear cystic.
Uterine Muscularis.
The three layers are not readily identified, but note again the large size of the fibers.
Note the huge multinucleated giant cells in the deep endometrium and especially in the muscularis. They are thought to be of trophoblastic origin (perhaps differentiated from but not to be confused with syncytial knots).
Slide 279. Placenta at term (H&E)[edit]
These slides are from a “fresh” placenta immediately after parturition; thus very little postmortem change is present and structures are seen distinctly.
Go over the fetal placenta as in slide 280. Numerous red blood corpuscles are present in the maternal blood spaces, probably due to rupture of blood vessels during parturition.
Note the tremendous vascularity of the placental villi, apparent here because of the fresh condition of the tissues; note also the great number of syncytial knots.
A fragment of decidua basalis may be present (left end of the section in the field). Anchoring villi are seen and large decidual cells may still be present.
Slide 274, Placenta at term (PASH)[edit]
This tissue is from the same placenta used for making slides 279 and 273. Look at the slide to see how term structures stain with PASH.
Basement membranes are prominent under the syntrophoblast and under endothelium of the blood vessels. Note also that blood vessels are more numerous in these villi than in those of slide 280, are also congested which may be the cause of their large size.
Areas of decidua basalis are present.
Slide 273, Placenta, term (Masson)[edit]
This tissue is from the same placenta as used for making slides 274 and 279.
Identify the structures as seen with this stain. Connective tissue elements are blue, nuclei are reddish or indistinct, and the cytoplasm varies.
This section shows the chorionic plate at the right (in the field).
The outer “membrane” is the amnion, consisting of a layer of cuboidal or low columnar epithelium and a thin layer of connective tissue. It is mechanically separated from the underlying chorion.
The chorion consists of a layer of connective tissue covered by syncytial trophoblast that is now mostly fibrinoid.
Two main umbilical vessels and smaller branches are passing through the chorionic plate.
Umbilical Cord[edit]
Slide 287, Umbilical Cords (H&E)[edit]
Slide 287, Umbilical Cords (H&E), is from an early pregnancy and from late in pregnancy.
The early pregnancy umbilical cord is on the left. The two umbilical arteries and the umbilical vein look generally similar because of the atypical large amount of muscle in the wall. An internal elastic membrane is lacking in the arteries. The diameter of the vein is greater than that of the artery and the muscle is not quite as compactly arranged.
The stroma of the cord is mucous connective tissue - embryonic connective tissue with a mucoid ground substance (Wharton’s jelly) which is removed in section preparation. Note the fine collagenous fibers and the large branched fibroblasts.
Covering the cord is simple squamous or simple cuboidal epithelium, part of the amnion.
Slides 287 (tissue on right) and Slide 277, umbilical cord at term (H&E)[edit]
In this fully developed placenta, the atypical structure of the arteries is well shown - a wide inner layer of longitudinally arranged muscle and a thick outer circular layer. Postmortem contraction causes collapse of the vessels. The vein has some inner longitudinal muscle; most of it is outer circular. Reticular fibers between muscle fibers are seen with H&E (due to postmortem shrinkage of muscle fibers). The small vacuoles are probably early degenerative changes.
Collagenous fibers in the stroma are somewhat heavier than in the earlier cord but are not mature fibers. Mucous connective tissue retains its embryonic nature; note that fibroblasts are still large branched cells.
Neutrophils are invading some areas of the stroma (lower field especially), also related to breakdown of the tissues.
Epithelium of the amnion surrounds the cord.
Slide 287, Umbilical Cord at term (tissue on right) (H&E)[edit]
Slide 277, Umbilical Cord at term (H&E)[edit]
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
A normal partial thromboplastin time is 28 to 37 seconds.