IPLab:Lab 6:PAN
Contents
Clinical Summary[edit]
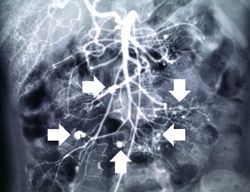
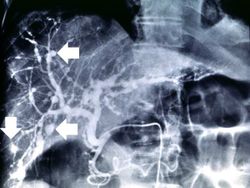
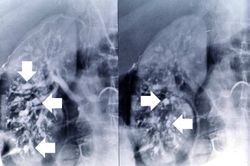
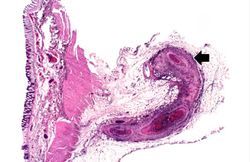
This was a 27-year-old white female who presented to the emergency room with fever, diarrhea, and abdominal pain that had increased in intensity over a 3-day period. Her blood pressure on admission was 165/108 mm Hg. She had been diagnosed with polyarteritis nodosa two years prior to this admission and had been treated with corticosteroids and cyclophosphamide. She had discontinued her corticosteroids because they made her gain weight; in addition, she was not taking the medications prescribed for her hypertension. At this admission it was suspected that the patient had bowel ischemia due to mesenteric artery occlusion. Angiographic evaluation revealed significant vascular damage to the mesenteric arteries with aneurysmal dilatations and thromboses. Significant vascular changes were also observed in the renal and hepatic circulation. On the second hospital day, the patient developed acute severe abdominal pain and an emergency laparotomy was performed to resect an 18-cm section of infarcted and ruptured ileum. After surgery she continued to run a fever, her white blood cell count was 13,500 cells/mm³, and she developed renal failure. Two days after surgery the patient died due to sepsis and multisystem failure.
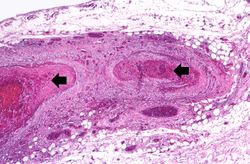
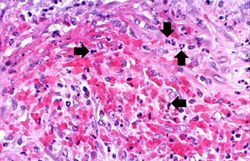
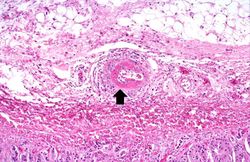
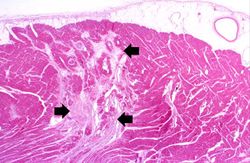
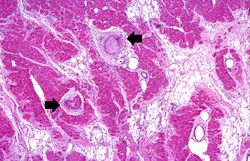
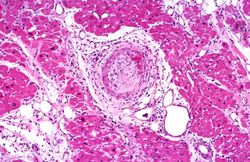
At autopsy there were several 0.5 to 1.0-cm firm nodules in the dermis. There were numerous aneurysmal dilatations grossly visible in the mesenteric arteries. There were multiple shrunken infarcts on the surface of the kidneys and the surface also had a fine granular appearance indicative of hypertensive renal disease. On cut section both the kidney and the liver had multiple firm white nodules.
Images[edit]
Virtual Microscopy[edit]
Study Questions[edit]
Additional Resources[edit]
Reference[edit]
- eMedicine Medical Library: Polyarteritis Nodosa
- eMedicine Medical Library: Wegener Granolomatosis
- Merck Manual: Polyarteritis Nodosa
Journal Articles[edit]
- Kaito Aoki, M.D., and Marenori Kojima, Ph.D. Polyarteritis Nodosa. NEJM 2024 390 (18)
- Morgan AJ, Schwartz RA. Cutaneous polyarteritis nodosa: a comprehensive review. Int J Dermatol 2010 Jul;49(7):750-6.
Images[edit]
A normal blood pressure reading would be 120/80 mm Hg.
An occlusion is a blockage.
A normal white blood cell count is 4000-11,000 cells/mm³.
Renal failure is the severe reduction of renal function and often leads to reduced urinary output.
An infiltrate is an accumulation of cells in the lung parenchyma--this is a sign of pneumonia.
The normal fibrinogen level is 184 to 412 mg/dL.