IPLab:Lab 6:Hashimoto's Thyroiditis
Contents
Clinical Summary[edit]
This was a 49-year-old woman who complained of tiredness and difficulty concentrating. She had gained weight over the last year and despite warm weather, she felt chilled without a sweater. Family history was significant for hypothyroidism in her mother and older sister.
On physical examination she had an enlarged thyroid gland with a firm, bosselated texture. Serum TSH was markedly elevated and antithyroid peroxidase antibodies were positive. These results supported the clinical impression of hypothyroidism; also, the texture of her thyroid gland and a positive family history suggested an autoimmune etiological factor. She was referred to an endocrinologist; however, before beginning treatment she died suddenly from a ruptured berry aneurysm.
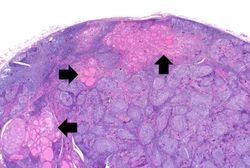
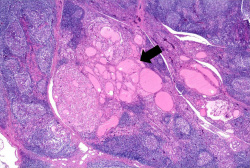
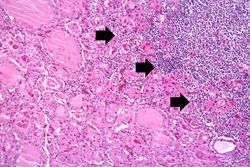
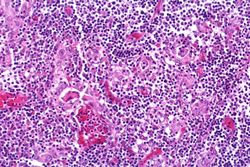
Images[edit]
Virtual Microscopy[edit]
Study Questions[edit]
Additional Resources[edit]
Reference[edit]
- eMedicine Medical Library: Hashimoto Thyroiditis
- eMedicine Medical Library: Hypothyroidism
- Merck Manual: Overview of Thyroid Function
- Merck Manual: Hashimoto's Thyroiditis
- Merck Manual: Hypothyroidism
Journal Articles[edit]
- Agrawal P, Ogilvy-Stuart A, Lees C. Intrauterine diagnosis and management of congenital goitrous hypothyroidism. Ultrasound Obstet Gynecol 2002 May;19(5):501-5.
Images[edit]
Related IPLab Cases[edit]
Bosselated means covered with rounded protuberances.
Autoimmune disorders involve an immune response directed at the host's own cells.
A berry aneurysm is a small saccular arterial aneurysm usually found at a vessel junction in the circle of Willis. These aneurysms frequently rupture, causing a subarachnoid hemorrhage.