IPLab:Lab 3:Acute Myocardial Infarction
Contents
Clinical Summary[edit]
This 78-year-old male experienced a posterior myocardial infarction six years prior to this admission. Recently, he had begun to experience occasional angina. Four days prior to death, he experienced anterior chest pain and discomfort which he regarded as not too distressing. However, EKGs showed a classic acute anterior myocardial infarction in addition to the healed posterior infarct. His bloodwork also showed an elevated troponin. The patient progressively deteriorated with signs of left ventricular failure and died with arrhythmias and pulmonary edema.
At autopsy his heart showed a healed posterior infarct. The right coronary artery was completely occluded but partially recanalized. The left main coronary artery had severe atherosclerotic stenosis and a thrombus filling the lumen. The entire anterolateral aspect of the left ventricle was soft with variegated areas appearing hyperemic or pale. There was extensive mural thrombosis and reactive pericarditis.
Images[edit]
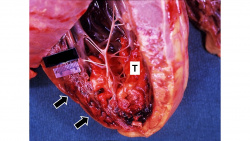
This is a gross photo of the heart at autopsy after the left ventricle was opened. Note the thrombotic material (T) that is present within the left ventricular lumen over the area of infarction. On the cut edge of the left ventricular free wall you can see the areas of hemorrhage and the pale myocardium indicative of an acute myocardial infarction (arrows).
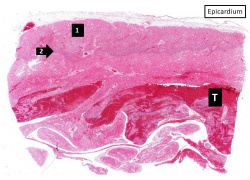
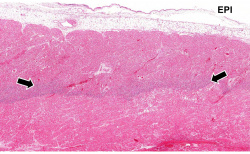
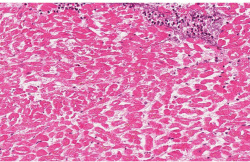
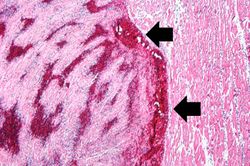
This is a low-power photomicrograph of infarcted heart. There is a layer of surviving myocardial tissue (1) along the epicardium and then a blue line (2) which represents the accumulation of inflammatory cells at the border of the infarct. There is thrombotic material (T) adherent to the endocardial surface.
Virtual Microscopy[edit]
Heart: Acute Myocardial Infarction[edit]
Normal Heart[edit]
Study Questions[edit]
Additional Resources[edit]
Reference[edit]
Journal Articles[edit]
- Helft G, Worthley SG. Anti-thrombotic, anti-platelet and fibrinolytic therapy: current management of acute myocardial infarction. Heart Lung Circ 2001;10(2):68-74.
Images[edit]
Related IPLab Cases[edit]
- Lab 1: Heart: Myocardial Infarction (Coagulative Necrosis)
- Lab 3: Heart: Healed Myocardial Infarction
- Lab 4: Heart: Mural Thrombus
- Lab 4: Coronary Artery: Thrombosis
- Lab 4: Lung: Pulmonary Congestion and Edema
Myocardial infarction is necrosis of myocardial tissue which occurs as a result of a deprivation of blood supply, and thus oxygen, to the heart tissue. Blockage of blood supply to the myocardium is caused by occlusion of a coronary artery.
Angina pectoris is chest pain produced by myocardial ischemia, it worsens upon exertion.
Arrhythmias are abnormal heart rhythms.
Pulmonary edema refers to the accumulation of fluid in the pulmonary alveolar and tissue spaces as a result of changes in capillary permeability and/or increases in capillary hydrostatic pressure.
Recanalization is the process of the forming of channels through an organized thrombus so that blood flow is restored.
A thrombus is a solid mass resulting from the aggregation of blood constituents within the vascular system.
Mural thrombosis is the formation of multiple thrombi along an injured endocardial wall.
Pericarditis is inflammation of the pericardium - often with deposition of fibrin.
Mural thrombosis is the formation of multiple thrombi along an injured endocardial wall.
An occlusion is a blockage.