IPLab:Lab 1:Myocardial Infarction
Contents
Clinical Summary[edit]
This was a 57-year-old male whose hospital course following abdominal surgery was characterized by progressive deterioration and hypotension. Four days post-operatively, the patient sustained an anterior myocardial infarction and died the next day.
At autopsy the patient's heart weighed 410 grams. Examination of the coronary arteries revealed marked atherosclerotic narrowing of all three vessels with focal occlusion by a thrombus of the left anterior descending artery. Fresh necrosis of the anterior wall of the left ventricle and anterior portion of the septum was present, extending from the endocardium to the inner half of the ventricular wall.
Images[edit]
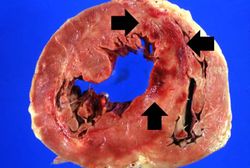
In this gross photograph of the heart from this case, note the area of fresh myocardial infarction (arrows) in the anterior portion of the left ventricle and extending into the anterior portion of the interventricular septum. Note that the walls of the left and right ventricle are slightly thicker than normal.
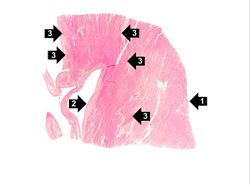
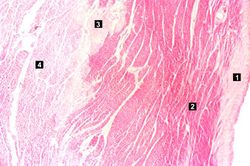
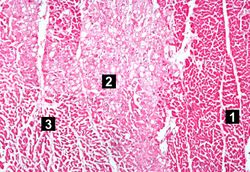
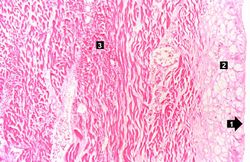
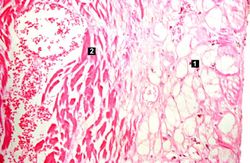
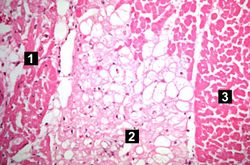
This higher-power photomicrograph shows endocardium on the right side of this image. Directly beneath the endocardium is a pale area consisting of cardiac myocytes exhibiting vacuolar degeneration (1). The area of infarction is visible as a hypereosinophilic area (2) and there is a second zone of vacuolated myocytes (3) between the infarct and the normal myocardium (4).
Virtual Microscopy[edit]
Myocardial Infarction[edit]
Normal Heart[edit]
Study Questions[edit]
Additional Resources[edit]
Reference[edit]
Journal Articles[edit]
- Agnew NM, Pennefather SH, Russell GN. Isofluorane and coronary heart disease. Anaesthesia 2002; 57(4): 338-347
Images[edit]
Related IPLab Cases[edit]
- Lab 3: Heart: Acute Myocardial Infarction
- Lab 3: Heart: Healed Myocardial Infarction
- Lab 4: Heart: Mural Thrombus
- Lab 4: Coronary Artery: Thrombosis
- Lab 4: Lung: Pulmonary Congestion and Edema
| |||||
Myocardial infarction is necrosis of myocardial tissue which occurs as a result of a deprivation of blood supply, and thus oxygen, to the heart tissue. Blockage of blood supply to the myocardium is caused by occlusion of a coronary artery.
Atherosclerosis is the deposition of lipid into the intima of arteries, resulting in narrowing of the vessel lumen.
An occlusion is a blockage.
A thrombus is a solid mass resulting from the aggregation of blood constituents within the vascular system.