Clinical Summary[edit]
For four months before death, this two-year-old black female infant ate poorly and lost weight. When hospitalized, she appeared chronically ill with signs of infection. An exploratory laparotomy showed the patient had enormously enlarged abdominal lymph nodes, the biopsy of which disclosed active histoplasmosis. Despite intensive therapy, the patient died three weeks after admission.
Autopsy showed widespread enlargement of lymph nodes, ulcers of the intestines, and enlarged adrenal glands exhibiting multifocal granulomas.
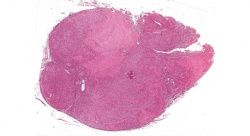
This low-power photomicrograph shows a section of adrenal gland with several irregularly-outlined areas of necrosis.
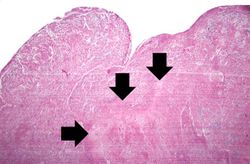
This higher-power photomicrograph of the previous adrenal gland shows more clearly the irregularly-shaped area of necrosis (arrows).
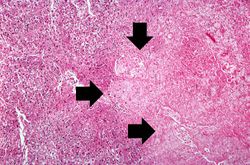
This is an even higher-power photomicrograph of an area of necrosis (arrows). There is loss of cellular detail within this area. There are inflammatory cells present; however, it is difficult to differentiate the inflammatory cells from the native lymphocytes of the adrenal gland--which is a lymph node.
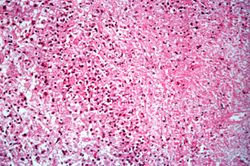
This high-power photomicrograph was taken at the edge of the area of necrosis. There is a mild inflammatory infiltrate along the edge of the necrosis.
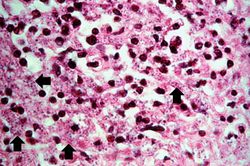
This high-power photomicrograph shows small (2-5 mm) dark-staining organisms in the cytoplasm of many of these cells (arrows).
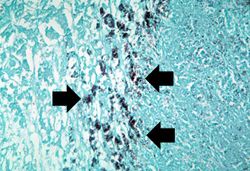
This is a high-power photomicrograph of the same section of tissue as the previous slide. This section, however, has been stained with methenamine silver which causes the Histoplasma organisms to stain black (arrows).
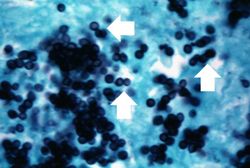
This photomicrograph was taken under oil immersion to show the silver-stained Histoplasma organisms. Some of the organisms appear to be budding (arrows).
Virtual Microscopy[edit]
Study Questions[edit]
Histoplasma capsulatum infection is usually acquired by inhalation of dust particles from soil contaminated with bird or bat droppings. The droppings contain small spores (microconidia).
1) A self-limited primary pulmonary involvement which may result in coin lesions on chest x-ray;
2) chronic, progressive, lung disease, which often localizes to the lung apices and causes cough, fever, and night sweats;
3) localized lesions in extrapulmonary sites, including mediastinum, adrenals, liver, or meninges; and
4) a widely disseminated involvement, particularly in immunosuppressed patients.
Histoplasma conidia and yeasts bind to the beta-chain of the integrins receptors LFA-1 (CD11a/CD18) and MAC-1 (CD11b/CD18).
Histoplasma yeasts are phagocytosed by the unstimulated macrophages, multiply within the phagolysosome, and lyse the host cells.
Additional Resources[edit]
Reference[edit]
Journal Articles[edit]