IPLab:Lab 13:Biliary Atresia
Contents
Clinical Summary[edit]
This eight-month-old female developed jaundice at one week of age. As the jaundice deepened, the child's bilirubin level was found to be over 30 mg/dL and the patient experienced a few convulsive episodes. A liver biopsy produced a diagnosis of extrahepatic bile duct obstruction. A subsequent exploratory laparotomy showed an absence of extrahepatic bile duct structures--including the gallbladder--and an intraoperative cholangiogram failed to show any large biliary channel. A jejunohepatostomy in the portal area was performed in the hope of establishing bile drainage and the patient was placed on the waiting list for a liver transplant. However, the patient progressively deteriorated, developed infections, and after a long turbulent course, died of pneumonia.
An autopsy was performed and the diagnosis of extrahepatic bile duct obstruction was confirmed.
Images[edit]
Virtual Microscopy[edit]
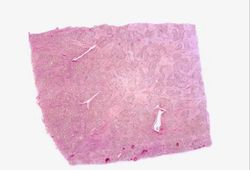
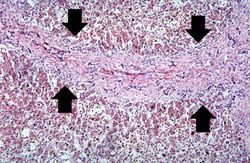
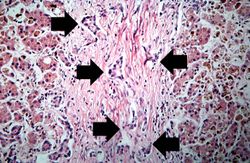
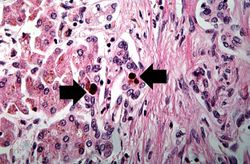
H&E[edit]
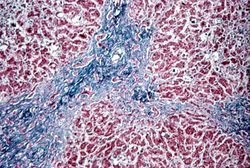
Masson Trichrome[edit]
Study Questions[edit]
Additional Resources[edit]
Reference[edit]
Journal Articles[edit]
- Davenport M, Caponcelli E, Livesey E, Hadzic N, Howard E. Surgical outcome in biliary atresia: etiology affects the influence of age at surgery. Ann Surg 2008 Apr;247(4):694-8.
Images[edit]
Related IPLab Cases[edit]
| |||||
Jaundice (or icterus) is a state of hyperbilirubinemia (increased bilirubin in the blood) in which bile pigment is deposited in the skin, mucous membranes, and scleras. This deposition of bile pigment results in a yellow appearance.
A normal bilirubin level for a child this age would be <2 mg/dL.
Transhepatic cholangiography involves the injection of a radiopaque dye into the intrahepatic ducts of patients with obstructive jaundice. Radiographs are then taken to determine whether a route exists for the dye to leave the liver.
A jejunohepatostomy is a procedure in which an attempt is made to bypass the biliary tree by having bile drain into the jejunum. Risks of this procedure include the development of bacterial infections of the intrahepatic biliary tree.
Liver transplantation (along with the donor's bile ducts) is the most successful treatment for these patients.
In alcoholics, aspiration pneumonia is common--bacteria enter the lung via aspiration of gastric contents.