IPLab:Lab 12:Acetaminophen Toxicity
Contents
Clinical Summary
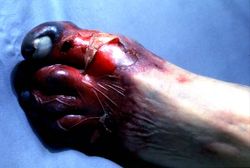
This 77-year-old white male with a past medical history of severe osteo- and rheumatoid arthritis went to his internist for increasing joint pain and was started on a new medication containing a narcotic analgesic, acetaminophen, and a non-steroidal anti-inflammatory agent. The patient also self medicated with acetaminophen. Two days later he went back to his doctor complaining of nausea and vomiting, right upper quadrant pain, anorexia, and confusion. Lab evaluation revealed massively increased liver enzymes. The patient went into DIC and died in fulminant liver failure.
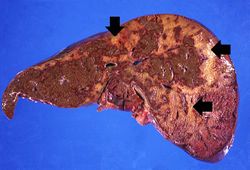
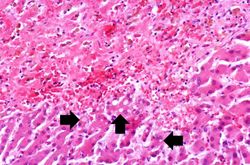
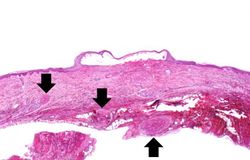
At autopsy the liver had large areas of pale softened tissue indicative of liver necrosis.
Images
Virtual Microscopy
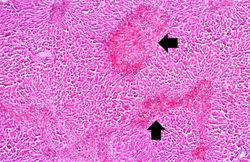
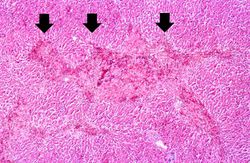
Liver: Acetominophen Toxicity
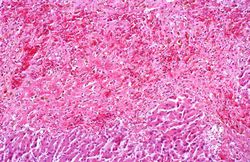
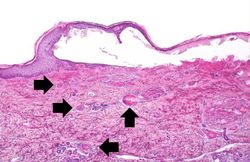
Normal Liver
Study Questions
Additional Resources
Reference
- eMedicine Medical Library: Acetaminophen Toxicity
- eMedicine Medical Library: Acute Liver Failure
- Merck Manual: Acetaminophen Poisoning
Journal Articles
- Schiødt FV, Lee WM, Bondesen S, Ott P, Christensen E. Influence of acute and chronic alcohol intake on the clinical course and outcome in acetaminophen overdose. Aliment Pharmacol Ther 2002 Apr;16(4):707-15.
- Yeates PJ, Thomas SH. Effectiveness of delayed activated charcoal administration in simulated paracetamol (acetaminophen) overdose. Br J Clin Pharmacol 2000 Jan;49(1):11-4.
Images
Related IPLab Cases
| |||||