Histologic:Chapter 14
Contents
Introduction[edit]
Anatomically and physiologically, the glands of the endocrine system share certain features in common:
- Ductless: The endocrine glands (glands of internal secretion) have no ducts (ductless) and pass their secretions directly into the blood or the lymphatic circulation.
- Produce hormones. Each endocrine gland produces and secretes chemical substances called hormones that selectively affect some target organ, either a group of tissues or the body as a whole. The target organ or tissue is stimulated, depressed or maintained by a particular hormone.
- Rich vascularization. Endocrine organs are very vascular, frequently with more than one source of blood supply. The blood supplies the energy for hormonal synthesis and via the close association of the blood vessels to the endocrine tissue, quickly and efficiently moves the hormones secreted into the blood to other parts of the body.
- Parenchyma and stroma. In most endocrine glands the parenchyma consists of epithelial cells, most commonly arranged as cords, which comprise the major portion of the gland. The stroma or connective tissue element of the gland consists of a few collagenous fibers with associated fibroblasts and reticular fibers and is generally sparse with respect to the parenchyma. Occasionally a lumen is found within the cords of cells such as in the zona glomerulosa of the adrenal cortex. A lumen is characteristically found in the follicles of the thyroid.
Classification of Endocrine Glands
Pure Endocrine Glands:
- pituitary
- thyroid
- parathyroid
- adrenal (suprarenal)
Mixed Endocrine Glands have an endocrine portion that produces hormones and an exocrine portion that produces non-endocrine products that pass out of the gland via a duct system.
The mixed glands include:
Pancreas
- pancreatic islets - secrete the hormones
- exocrine portion - secrete the digestive enzymes
Ovaries
- granulosa (follicular) cells theca lutein cells - secrete hormones corpus lutein cells
- cytogenic portion - concerned with maturation and release of ova
Testes
- interstitial cells (of Leydig) - secrete hormones
- cytogenic portion - involved with maturation and release of sperm
Placenta
- syncytiotrophoblast cells - secrete hormones plus regulate selective absorption of nutrients and excretion through fetal placenta
Endocrine functions of incidental nature
- Liver
- Stomach
- Small intestine
- Kidney
Other endocrine glands:
- Specific hypothalamic neurons (secrete pituitary releasing factors)
- Pineal body
- Paraganglia
- Thymus
Pituitary Gland (Hypophysis)[edit]
The term “master gland” is frequently applied to the pituitary gland because its hormonal secretions control essential body functions such as body growth, sexual development and maturation and reproduction and regulate the activities of the adrenals and thyroids.
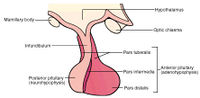
The pituitary gland is of dual origin, being derived partly from Rathke’s pouch, (the embryonic invagination of ectoderm of the oral cavity) and partly from an invagination (diverticulum) of the diencephalon brain wall (neural ectoderm). Anatomically, there are two gross divisions of the pituitary gland:
- Anterior lobe (adenohypophysis) - major portion of gland (about 75% of total pituitary gland).
- Posterior lobe (neurohypophysis) - connected to hypothalamus via infundibular stalk containing the bundle of unmyelinated nerve fibers, the hypothalamic-hypophyseal tract.
Embryologically, the major divisions of the pituitary gland are the adenohypophysis (the glandular epithelial part of the pituitary gland) and the neurohypophysis (the neural portion of the pituitary gland).
Adenohypophysis (3 subdivisions):
- Pars distalis (anterior lobe) - major subdivision of the pituitary gland. Pars distalis is derived from the rostral wall of Rathke’s pouch.
- Pars tuberalis - minor subdivision of the pituitary gland. Pars tuberalis is an upper extension of the distalis and forms a sleeve or collar around the infundibular stalk.
- Pars intermedia - another minor subdivision of the pituitary gland. Pars intermedia gets its name from the fact that it is located intermediate between the adenopituitary gland and the neurohypophysis.
Neurohypophysis (2 subdivisions):
- Pars nervosa (infundibular process, neural lobe)
- Infundibulum
Infundibular stem
Median eminence (of the tuber cinereum)
There are three slides of the pituitary gland: 201(PASH), 202(Mallory), and 203(H&E). The latter shows some of the general features of the pituitary gland; the Mallory-stained specimen is for detailed histology, particularly of the pars distalis; the PASH slide is for histochemical analysis of hypophyseal function.
Slide 203, Hypophysis (H&E)[edit]
Slide 203 (H&E) shows at least three of the important anatomical-physiological areas of the pituitary gland: the pars nervosa, pars intermedia and pars distalis. Dura mater surrounds the pituitary gland; it may be mechanically separated or torn in places.
In the pars distalis, using lower magnifications, scan the entire organ. Notice that certain areas have clusters (actually cords) of cells staining faintly blue, while in other areas, groups of reddish-staining cells will be seen. At 40x power note how these clusters or cords of cells are separated from another by blood-filled spaces called sinusoidal capillaries. The cells rest on a basement membrane, but in sections they are often detached from it, the result of post- mortem change in the tissue.
Identify acidophils, large cells filled with prominent, eosinophilic granules.
Chromophobes are small cells with pale or faintly staining cytoplasm and distinct cell outlines. They occur in groups, interspersed between other cell types.
Basophils are the least numerous, are of varying sizes, have lightly basophilic cytoplasmic granules that vary in amount in different cells, and have distinct cell outlines. These are not easy to identify with H&E stains.
Pars nervosa looks like a mass of connective tissue with fibroblasts. Actually, the cells are pituicytes (modified neuroglia cells) with rounded or oval nuclei and a small amount of cytoplasm, not usually distinguishable because of shrinkage. Elongated cytoplasmic processes of pituicytes form the fibrillar appearing meshwork of the pars nervosa. Blood vessels are supported by true connective tissue; occasional small septa may be present (seen better with Mallory’s stain).
Look for Herring bodies, seen better here than in the other two slides. The Herring bodies are circular to irregularly circular structures filled with light-to- dark blue or brownish granules of various sizes and are usually but not always located near blood vessels. Recall that Herring bodies represent accumulated neurosecretory material (ADH and oxytocin) in the supraoptic and paraventricular nuclei of the hypothalamus.
The pars intermedia can be seen with the naked eye or with scanning lens, as that area of the section distinguished by the prominently staining bright red colloidal-filled vesicles (running vertically and separating the light-staining pars nervosa from the darker-staining pars distalis).
Slide 202, Pituitary Gland (Mallory)[edit]
On slide 202, Pituitary gland (Mallory), the tissue is cut in such a fashion that (1) most of the pituitary gland consists of pars distalis (2) a small wedge or cone of pars nervosa is present in the inferior mid-line region of the section and (3) a small area of pars intermedia can be seen immediately above the pars nervosa region. Dura is present.
Scan at low magnification and observe that the pars distalis makes up most of the section. The pars distalis can be identified by the presence of anastomosing cords of cells separated from sinusoidal capillaries by small amounts of blue-staining connective tissue fibers. At this magnification, identify the pale area containing prominent blue-staining strands of connective tissue. This area is the pars nervosa (actually, only a very small part of it). Adjacent to the pars nervosa, note the large cyst-like structures filled with blue or reddish-purple colloid material. This is the area of the pars intermedia. Extending above this area is a narrow blue-staining region surrounded on either side by the pars distalis. This blue area is an artifact of fixation and staining: it represents pars distalis that failed to stain acidophilic.
At higher magnification, note again the cords of cells (50 to 70 micrometers wide) that make up the bulk of the pars distalis and the sinusoidal capillaries (35 to 40 microns in width) that are present on either side of the cords. At 40x power, note the small amount of stroma containing a few fibroblasts and a few macrophages (fixed) that are not readily identifiable. There is considerable variability in the cell types making up the cords. Identify in different areas:
The chromophobes - cytoplasm is almost colorless and has no apparent granulation. Cell boundaries are indistinct or invisible. The chromophobes tend to be centrally located in the cords. At 10X scan the whole pars distalis and note that these cells (chromophobes) make up about half the cells. The chromophobes are the smallest of all cells in the pars distalis and are generally regarded as degranulated chromophils. During pregnancy, some of the chromophobes develop acidophilic granules and are referred to as “pregnancy cells.”
The chromophils - comprise the remaining half of the cells in the cords of the pars distalis. These cells have a marked affinity for the ingredients of the Mallory stain. Two groups of cells make up the chromophils:
Acidophils (alpha cells) consist of (a) somatotropes - the source of growth hormones (GH) or (STH) and (b) mammotrophs (LTH) which synthesize prolactin. They contain carmine or orange-colored granules in their cytoplasm and constitute about 37% of the epithelial cells of the pars distalis.
Basophils (beta cells) - the source of FSH, TSH, LH (ICSH) and possibly ACTH. They are larger and more irregular in shape than acidophils; found predominantly in the periphery of the anterior lobe and constitute about 13-15% of the cells of the pars distalis. The beta cells contain blue to purplish-blue granules and may have minute vesicles in their cytoplasm. With more refined staining the numbers and types of cells differ considerably.
In the pars intermedia, note that the few cavities or vesicles present are filled with blue or reddish-blue colloid. At higher magnification, these vesicles are lined by squamous to simple cuboidal basophilic epithelial cells.
In the pars nervosa, this stain reveals only a few blood vessels, some small septa of blue-staining connective tissue fibers and a background of lightly staining fibrillar or flocculent-appearing material that represents the unstained processes of pituicytes and unmyelinated nerve fibers.
In general, neither pituicytes nor Herring bodies are stained.
Slide 201, Pituitary Gland (PASH)[edit]
On slide 201, Pituitary gland, pars distalis only, (PASH), the section is stained for carbohydrate moieties by PAS and counterstained with H (hematoxylin).
First scan the slide at low power. At this magnification the PAS staining outlines of the sinusoidal capillaries are very distinct. What portion of the sinusoidal capillaries is being stained by PAS? Also note that in one part of the pars distalis, a large blood vessel surrounded by considerable connective tissue appears to have many sinusoidal capillaries radiating from it; this particular blood vessel may not be on all slides. The pars nervosa does not appear to be present; the pars intermedia is difficult to distinguish; few, if any colloid-filled vesicles are present.
At medium power, observe where the bright red PAS staining cells are located. These are basophils that take up the red of the PAS. At high power, basophils are filled with bright-red PAS staining granules or with less reddish staining granules. Neither acidophils nor chromophobes take up the PAS stain; the cytoplasm remains either colorless or slightly tinged with purple granules. The nuclei of both the PAS-stained and non-PAS-stained cells are equally prominent, with a clear or definitive nuclear membrane.
Thyroid[edit]
The thyroid consists of two separate lateral lobes and a connecting part, the isthmus, lying over the superficial part of the trachea just below the larynx. Embryologically, the thyroid is derived as a diverticulum (thyroid diverticulum) from the midventral floor of the pharynx (entoderm).
The thyroid develops very early and is present as a diverticulum in the human embryo before the end of the first month of gestation. The embryonic thyroid is at first attached to its point of origin by the thyroglossal duct located at the root of the tongue. The attachment of the duct to the tongue is marked by a pit, the foramen caecum, present in the root of the adult tongue. During development, the thyroglossal duct regresses, but remnants may persist as thyroid tissue within the tongue (lingual thyroid), as thyroglossal duct cysts, or as the pyramidal lobe of the thyroid.
The thyroid has a very rich blood supply with autonomic nerves innervating the vessels to regulate blood flow through the gland (see anatomy text for details). It is important to emphasize that the thyroid gland is very labile and varies in size and structure in response to such factors as sex, nutrition, age, season, temperature and the iodine content of food.
The thyroid is surrounded by a capsule of fibroelastic tissue that is continuous with the surrounding peritracheal fascia. The capsule sends septa into the gland, dividing it into lobules. The connective tissue septa support the parenchyma and carry blood vessels, lymphatics and nerves. Each lobule is composed of characteristic structural units of the thyroid gland known as follicles.
Human thyroid follicles (estimated to number about 3 million in the whole thyroid) vary greatly in shape and in size. Each follicle is the result of secretory activity of the simple epithelium of glandular cells that line its lumen. The follicular cavity becomes filled with colloid, a semi-fluid, homogenous substance rich iodine and the depot of the storage form of the active thyroid hormones. In the state of normal activity (euthyroid), the lining epithelium of the follicle is simple cuboidal or low columnar. The interfollicular areas contain highly vascular fibrous connective tissue that separates one follicle from the next. Generally when the gland is in a resting state, the follicular cells are simple squamous. Their secretions are released into the follicular lumen, resulting in a large lumen containing an increase in the content of colloid.
When the gland is active, the epithelium is of a tall columnar type that shows a tendency to fold upon itself. In such cases, the active hormone passes from the colloid in the lumen to the follicular cells and then into the capillaries. If the gland is highly active, the secretions from the follicular cells go directly into the capillaries.
Thyroxin T4, tetraiodothyronine, is the principal circulating hormone of the thyroid gland while tri-iodothyronine (T3), although present in much lower concentration, is much more potent than thyroxin. Both of these hormones are the result of follicular cell synthesis regulated by the circulating level of TSH. The follicles actually contain two different cell types. The predominant one, the follicular cell (principal cell) is responsible for the two thyroid hormones (T3 and T4). In the interfollicular area and interspersed among the follicular cells (but not next to the lumen of the follicle) are scattered groups or single cells called parafollicular cells (light cell, C-cell). The latter names refer to their paler cytoplasm. These cells are larger than the follicular cells. They are found in thyroids of the dog and rat; they are less identifiable as such in the human thyroid. The function of the parafollicular cells is to secrete calcitonin, a hormone that lowers blood calcium levels counteracting the effect of the parathyroid hormone (PTH).
Slide 207, Thyroid (H&E)[edit]
On slide 207 Thyroid, (H&E), use low power to observe the many small round to irregular shaped follicles that occupy almost the entire section. Note how the follicles are grouped into larger structures, the lobules. The latter are often demarcated by the presence of considerable connective tissue containing blood vessels. (Much of the connective tissue has been torn out during slide preparation.) A capsule is not present.
With higher magnification, note that the follicles are filled with pink-staining colloidal material. Observe the height of the follicular cells. Examine several follicles in various regions of the section; note that the cells vary from cuboidal to columnar or even squamous. Not all follicles are lined by identical height or size of follicle cells; sometimes the same follicle may show differences from one side of the follicle to the other with respect to follicular cell dimensions. The smaller the follicle the more cuboidal or low columnar the cells become. In some of the interfollicular areas, note very small follicles beginning to form; very little if any colloid is contained in these follicles. This thyroid came from a younger individual and displays moderate activity.
Sinusoidal capillaries between follicles are difficult to distinguish because of postmortem change and contraction of tissues; occasional endothelial nuclei can be identified.
Look for parafollicular cells in the walls of follicles or in the interstitial tissue close to the follicles; these are also difficult to distinguish.
Slide 206, Thyroid (H&E)[edit]
Note at low power that most of the follicles are much larger than in slide 207. This tissue came from an older individual.
With higher magnification, examine the follicular cells from follicles selected at random and notice that most are lined by squamous cells. Does the overall appearance of this thyroid specimen represent an active thyroid?
Parathyroid[edit]
In most individuals there are four parathyroid glands lying on the dorsal portion of the thyroid, embedded in a true capsule, thus separate from the thyroid. Ectopic parathyroids may be found anywhere from the base of the skull to the arch of the aorta, specifically in the thymus, in the cervical area external to the thyroid and in the mediastinum. The parathyroids have a rich blood supply although not as extensive as the thyroid. Developmentally, the superior pair of parathyroids forms from the endodermal 4th pharyngeal pouches (these parathyroids referred to as parathyroids IV); the inferior pair develop from the 3rd pharyngeal pouches (parathyroids III), as does the thymus. This fact explains the ectopic or aberrant occurrence of parathyroids in the thymus.
Each parathyroid consists of densely packed groups of anastomosing cords and clumps of cells separated by a rich network of large sinusoidal capillaries. Thin connective tissue septa penetrate the gland but do not divide it into distinct lobules. Two types of epithelial cells are observed: chief or principal cells and oxyphil cells. The chief cells are believed to be the source of the only hormone synthesized by the parathyroid, parathyroid hormone (PTH). PTH functions to regulate the level of calcium and phosphorus in the blood by affecting the metabolism of those cells involved in the intake, secretion and deposition of calcium in the body. There is no evidence for pituitary control over parathyroid activity; no parathyroid trophic factor has been isolated. The parathyroid glands are essential for life. Their complete removal in most mammals is fatal.
Slide 211, Parathyroid (H&E)[edit]
Identify the two types of parenchymal cells, the chief cells and oxyphil cells.
The chief cells predominate; they are characterized by having large vesicular, centrally located nuclei. The cytoplasm does not stain uniformly.
Some chief cells are darker than others. An occasional chief cell may show water-clear cytoplasm, apparently “empty.” PAS-stained preparations of parathyroid demonstrate varying amounts of glycogen deposited in the cytoplasm of the chief cells.
The oxyphil cells are scattered among the chief cells; they occur singly, in clusters or nests and they are much fewer in number than the chief cells. Oxyphils are larger than chief cells, have an acidophilic (eosinophilic) finely granular cytoplasm and a small, dark, somewhat pyknotic nucleus. Observe the well-defined cell outline of the oxyphil cells.
Since oxyphil cells do not appear until immediately prior to or at the time of puberty and gradually increase in number as one gets older, the current consensus is that oxyphils and other cell types (transitional cells identifiable by EM) represent modifications of the chief cell.
Recent EM observations tend to favor the concept that there is only one parenchymal cell type, the chief cell.
Note the rather loose, delicate connective tissue in which are contained blood vessels of varying sizes. It is difficult to identify well-defined connective tissue septa that invade the organ from the capsule to supply it with nerves, blood vessels and lymphatics.
Fat cells are not as numerous in this preparation as in many sections of parathyroid.
An occasional colloid-filled vesicle may be observed on some slides.
Suprarenal (Adrenal) Glands[edit]
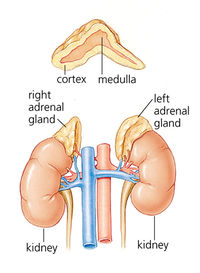
The suprarenal glands (adrenal glands) are one of the major homeostatic organs of the mammalian body. They are composed of two separate endocrine organs that differ in embryological origin, type of secretion and function. In mammals, the two organs are arranged as an outer cortex and an inner medulla surrounded by a common capsule.
Developmentally, the adrenal cortex arises from coelomic mesoderm (mesothelial cells) located between the urogenital fold and the dorsal mesentery. A portion of the gonads also arises from the same mesodermal source. The adrenal medulla is derived from neural crest ectodermal cells that invade the developing cortical tissue during the 2nd month of development. The suprarenal glands are highly vascular; more blood passes through these glands in relation to their size than through any other organ of the body, with the exception of the thyroid. The major blood supply is from the superior suprarenal arteries (branches of the inferior phrenic artery), which together with two other arterial sources form an arterial plexus in the suprarenal capsule from which three intraglandular vessels arise.
The adrenal cortex comprises about 90% of the total volume of the suprarenal gland, the medulla the remaining 10%. The cortex, whose secretory rate is controlled by hormones of the adenohypophysis and kidney, produces steroid hormones that affect protein and carbohydrate metabolism, resistance to physiologic stress and electrolyte distribution. The medulla, under nervous control, secretes catecholamines that affect heart rate and smooth muscle function in blood vessels and other viscera, as well as influencing carbohydrate and lipid metabolism. The cortex is essential for life; if destroyed or rendered ineffective, replacement therapy using its primary steroids will maintain life. The medulla, on the other hand, is not essential for life.
The adrenal cortex can be divided into three structural subdivisions or concentric zones.
The zona glomerulosa is the outer zone immediately beneath the capsule. It accounts for 15% of the total cortical volume.
The zona fasciculata occupies the middle zone. It comprises about 78% of the total cortex and thus, it is the widest zone.
The zona reticularis makes up about 7% of the total cortical volume. As the innermost zone it lies adjacent to the medulla.
During in utero development, a large 4th zone is present in the adrenal cortex: the fetal cortex (fetal zone), which lies next to the medulla. The fetal cortex constitutes approximately 80% of the cortex at birth, but it undergoes rapid involution or degeneration after birth while the definitive or permanent cortex enlarges to eventually become differentiated into the familiar 3 zones of the adult gland (by the 3rd year). The fetal adrenal is under the control of ACTH secreted by the pituitary gland of the fetus. The human fetal adrenal gland is a steroidogenic organ forming part of the “fetal placental” unit.
The majority of the cells of the adrenal medulla are called chromaffin cells because these cells display the brown “chromaffin reaction” color when the tissue is fixed in chromic acid or potassium dichromate. Catecholamines contained in the granules of chromaffin cell cytoplasm, when oxidized, account for this color reaction. Catecholamines also form a yellow-green fluorescent compound after reacting with formaldehyde, a technique that has proven valuable recently in mapping the distribution of catecholamines in the adrenal medulla and in the nervous system. The chromaffin cells are also referred to as the pheochrome cells or pheochromocytes (because of their dark staining reaction with chromic acid), and give rise to the tumor, pheochromocytoma.
With appropriate histochemical techniques, two types of chromaffin cells can be distinguished: the: the norepinephrine cells and epinephrine cells, the cells of origin of the two catecholamines of the medulla; norepinephrine and epinephrine, respectively.
Slide 215, Suprarenal Gland (Adrenal), (H&E)[edit]
Observe that the cortex completely surrounds the medulla. The medulla is distinguishable from the cortex by being more basophilic (a bluish-purple). The outer margin of the cortex also stains dark blue, which upon higher magnification will be seen to be the zona glomerulosa.
Scan the entire section. Note the thick capsule and external to it blood vessels of different sizes that are located in the suprarenal fat pad.
Identify several connective tissue trabeculae coming off the capsule and descending into the cortex partway; these trabeculae contain longitudinal sections of blood vessels, but they are not prominent. Blood vessels are also seen in various regions of the capsule in both longitudinal and cross-sections.
Identify the three zones of the cortex: they are the zona glomerulosa, zona fasciculata and zona reticularis. On this slide the zona glomerulosa is not uniformly thick, nor is the whole cortex since the plane of section may not be vertical to the surface in all areas. Note in some areas the cells in the zona glomerulosa are arranged as ovoid groups containing a tiny lumen, whereas in other places the cells show a somewhat haphazard arrangement.
Examine the different zones with high power and note the appearance of the cytoplasm and the size of the cells. Observe the vacuolated appearance of the cytoplasm of the zona glomerulosa versus the more acidophilic, vacuolated appearance of the zona fasciculata cell cytoplasm. These latter cells are sometimes called spongiocytes because of their vacuolated cytoplasm. The cytoplasm of the zona reticularis appears to be slightly more basophilic, although still vacuolated. The vacuolations in the cells of the cortex occur when lipid material dissolves from the tissue in preparing the section.
Compare the size of the cells of the fasciculata zone with those of the reticularis and glomerulosa. The fasciculata cells are somewhat larger.
Sinusoidal capillaries are clearly seen in the zona reticularis (either empty or filled with blood cells), but they appear to be collapsed in the zona fasciculata region; their presence is marked by the thin, dark ellipsoid nuclei of the endothelial cells that line them. The sinusoidal capillaries of the zona reticularis open directly into collecting vessels in the medulla. The functional significance of this anatomical relationship should be obvious: cortical secretory products can pass directly to the medulla to affect its activity.
Examine the somewhat spongy and more irregularly arranged medulla. The cells are polyhedral in shape; they have basophilic cytoplasm and fairly large, vesicular nuclei. Postmortem changes in the tissue of this section account for the poor staining characteristics of the chromaffin cells and their irregularly shrunken appearance. When optimally obtained and fixed, the medullary cells are seen to be larger and more granular than those of the cortex. Note the outlines of connective tissue fibers surrounding the cords of chromaffin cells. Such supporting fibers are better delineated on slide 216.
Recall that the medulla has a direct arterial blood supply which passes through the cortex as arterioles and breaks up into capillaries within the medulla. The medulla also receives blood by way of the sinusoidal capillaries leaving the zona reticularis as mentioned previously. Identify venules of various sizes; these are branches of the central medullary vein that is present on some slides. It has connective tissue and muscle in its wall. On Slide 215 can be seen longitudinal bundles of smooth muscle in the medullary vein. This vein emerges from the gland as the suprarenal vein.
Sympathetic ganglion cells occur in the medulla of the suprarenal gland, but they are difficult to identify on these slides.
Slide 216, Suprarenal Gland (Masson)[edit]
Slide 216, suprarenal gland (Masson), was obtained from a monkey and is superior to the other two slides in that less postmortem changes took place prior to fixation.
- Note the distinct capsule, stained blue, and sending delicate trabeculae (few in number) into the gland.
- Observe outside the capsule blood vessels, nerves and suprarenal adipose tissue.
- Compare the various zones of the cortex and the histological features of the medulla. Note the almost uniform thickness of the zona glomerulosa, the well-defined reticular fibers outlining the sinusoidal capillaries in the zona fasciculata and the very thick zona reticularis (not characteristic of the human adrenal).
- Some of the wide, irregular spaces in the reticularis zone are artifacts created when the section was spread on the slide and torn apart.
- In the zona reticularis and the zona fasciculata, the nuclei are differentially stained either a reddish or bluish color. The significance of this differential nuclear staining is not known.
- Large, longitudinally arranged sinusoidal capillaries can be seen in a few areas of the reticularis zone. Some may be filled with blood cells.
- The outlines of some of the chromaffin cells show varying amounts of basophilic granulations in the cytoplasm. Some medullary cells have a clear dark-purple cytoplasm and well-defined cell membranes.
- Note the medullary vein and its tributaries; the latter are venules with minimal connective tissue in their walls. The medullary vein may have a wider zone of connective tissue.
Endocrine Pancreas (Pancreatic Islets of Langerhans)[edit]
Small nests or islands of cells, isolated from the exocrine elements only by delicate reticular fibers, collectively form the structural basis of the vital endocrine elements of the pancreas. The secretions of these nests, the pancreatic islets (of Langerhans), are extremely important for normal body utilization of carbohydrates. The islets have no duct system: their products, like those of other endocrine glands, are released directly into the circulatory system.
With clusters of a few to hundreds of cells in each islet, the total number of islets in the human pancreas is estimated to be approximately 1 million, with the tail of the pancreas containing the greatest concentration of islets. Occasional single islet cells may be found among the exocrine secretory cells of the pancreatic acini. Within each islet, the cells are arranged as irregular cords, separated from each other by a rich and irregular distribution of blood capillaries. Every endocrine cell in the islet is in contact with a capillary, which emphasizes the highly vascular nature of islet tissue. In contrast, the acinar tissue is less well supplied with capillaries.
Two cell types make up almost the entire population of each islet, alpha or α-cells and β-cells. By far, the most numerous are the β-cells (60 to 90%) which are found in the interior of the islet and produce insulin; while the α-cells tend to occupy the periphery of the islet and contain glucagon. Both cell types are difficult to tell apart with routine H&E staining. In man, EM pictures of the β cell granules show that they consist of dense crystalloid structures in a pale homogenous matrix, enclosed within a loosely fitting limiting membrane. The β-cell cytoplasm contains more rough endoplasmic reticulum and free ribosomes and a more prominent Golgi complex than is the case for the α-cell. The α-cell’s secretory granules are spherical with the membrane more closely adhering to the dense core. With aldehyde fixation, a less dense matrix fills the space between the dense core and the membrane sac. The α-cell has more endoplasmic reticulum than the β-cell. The δ-cell usually has larger granules than α or β cells. Somatostatin is a product of the δ-cells.
Slide 154, Pancreas (H&E)[edit]
The islets are set apart from the acinar tissue by a thin fibrous membrane with flattened fibroblasts, which is not always seen as a continuous structure. The cords of islet cells are supported by minimal connective tissue in which course the capillaries. In sections of single islets, β-cells are predominant or may appear to be the only cell type present.
Scan the slide to see the large number of islets of varying sizes; this tissue is probably from the tail of the pancreas. Observe the cells, capillaries, connective tissue within the islets, and the thin connective tissue membrane around the islets.
With high magnification see if you can identify α & β-cells. The β-cells have distinct, lightly-staining granules, loosely arranged, and indistinct cell boundaries. The cytoplasm of α-cells is filled with fine granules so that it may look homogeneous; they stain pink with eosin.
The cell membrane is well defined and the nucleus may be darker (but not always).
Slide 155, Pancreas (Mallory stain)[edit]
Islets are not as numerous as in slide 154.
The section is somewhat overstained. The cytoplasm of α-cells appears homogeneous and has a brownish color, quite distinct from the loose arrangement of cytoplasm granules of β-cells. Rarely a δ-cell may be seen; its cytoplasm has an intense bright blue stain.
Identify other features of islets as above.
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
The normal fibrinogen level is 184 to 412 mg/dL.