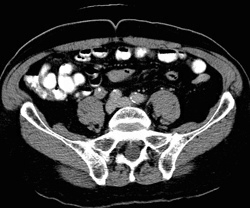
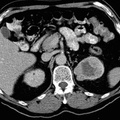
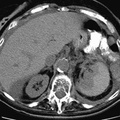
RADIOLOGY: KIDNEY: Case# 32990: RIGHT URETERAL TCC, LEFT RENAL CELL CA. 79 year old man with hematuria. There is a large, heterogeneous enhancing mass in the upper pole of the left kidney. There are several cysts within the lower portion of the left kidney. The right kidney shows heterogeneous enhancement in the anterior aspect of the right kidney in the mid to upper portion. There is a stent extending from the right renal pelvis into the bladder. The distal ureter is thickened at the level of the sacrum with soft tissue density around the stent. There is no abdominal or pelvic adenopathy. 85% of renal neoplasms are renal cell carcinomas, most commonly occurring in men, at ages 50-70, and usually involving one kidney. Only 2% are bilateral. Metastases are present at the time of diagnosis in 40% of cases. Since surgery is the only cure, early detection and accurate staging are important. The most common CT finding is a solid mass although low density areas due to hemorrhage or necrosis may be present. Cystic and multicystic forms may be seen. Stippled central or "eggshell" peripheral calcifications are seen in 10%. These tumors are usually hypervascular which may be evidenced by the presence of tortuous vessels in the perirenal fat. Tumor growth into the renal vein occurs in 30% of the time and into the inferior vena cava 5-10%. Venous invasion does not preclude surgical resection, but its identification is crucial to surgical planning. Renal cell carcinomas may spread locally to perirenal fat and adjacent organs. This is seen as strand or nodules of low density. Enlargement of renal hilar, pericaval, and periaortic nodes to 15mm or more indicates lymphatic spread. Hematogenous spread to the lung, bone, liver, adrenals, and the opposite kidney may occur. Distant metastases occasionally disappear with the removal of the primary tumor. Late appearance of metastases as long as 20 years following "cure" is also seen. Uroepithelial tumors account for 5 to 10% of renal tumors. 85% of these are transitional cell carcinomas while the remainder are usually squamous cell carcinomas. Hematuria is common, and these tumors usually present earlier than renal cell carcinomas. Most transitional cell tumors have a papillary growth pattern and are attched to the mucosa by a stalk. Non-papillary tumors are flat or nodular and usually agressive. They more commonly cause strictures in the collecting system and ureters. CT typically shows a low attenuating (15-30H) soft tissue mass within the renal pelvis or renal sinus, distorting and compressing the collecting system. Transitional cell carcinoma is readily differentiated from renal calculi on CT images since its numbers are much less than even radiolucent calculi (150-200H). Metastases to liver, lung, and bone occur, and multiple tumors are common. Patients with upper pole tumors have multicentric tumors in 20-44% of cases, and those with TCC of the ureter develop TCC of the bladder in 20-37% of cases.
- Author
- Peter Anderson
- Posted on
- Thursday 1 August 2013
- Tags
- adrenal hemorrhage, kidney, radiology
- Albums
- Visits
- 2018
0 comments