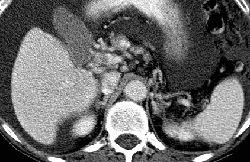
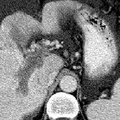
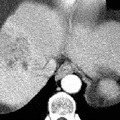
RADIOLOGY: HEPATOBILIARY: Case# 32827: CIRRHOSIS, CAVERNOUS TRANSF., PVT, HCC. The patient is a 71 year old man with known hepatocellular carcinoma. Study is for follow-up. There is a gross amount of ascites within the abdomen and pelvis. This surrounds the liver and spleen, lies within loops of bowel in the mesenetery and forms a large pool in the pelvis. In the liver, there is an heterogeneous, ill-defined mass in the dome of the liver which involves the medial segment of the left lobe and anterior segment of the right lobe. In addition, there is thrombosis of the main, right, and left portal veins with cavernous transformation evident. The configuration and contour of the liver is consistent with cirrhosis. Several small retroperitoneal varices are noted. In the United States, eighty percent of hepatocellular carcinomas arise in cirrhotic livers. Hepatocellular carcinoma usually appears as a hypodense or isodense lesion on nonenhanced images and enhances prominently during the arterial phase on dynamic contrast injection. Areas of tumor necrosis and calcification are common. Tumor invasion of hepatic and portal veins occurs frequently causing thrombosis of these vessels. Portal vein thrombosis may be accompanied by portal hypertension and its manifestations such as formation of collaterals, splenomegaly, and ascites. Portal vein thrombosis is readily diagnosed by CT and is best visualized with the incremental dynamic imaging technique. Acutely, the involved vessel enlarges, and the vessel wall may appear thickened and enhanced. There may be a small amount of contrast passing around the thrombus. The vessel itself has a relatively low central density. Serial examinations may show a change in the location or extent of thrombus, recanalization of the vessel, or retraction of the thrombus with collateral vein enlargement. Evidence of cavernous transformation of the portal vein may be seen as marked dilation of the periportal collaterals. This is caused by enlargement of extensive collaterals around the portal vein as a result of longstanding portal vein thrombosis and portal hypertension, resulting in obliteration of the portal vein.
- Author
- Peter Anderson
- Posted on
- Thursday 1 August 2013
- Tags
- hepatobiliary, radiology
- Albums
- Visits
- 798
0 comments